|
Are you tired of dealing with uncomfortable vein issues? Are varicose veins or spider veins causing you discomfort or embarrassment? If so, Total Vein Care in Fort Collins has a solution for you: Endovenous Vein Ablation. This innovative treatment is revolutionizing the way we address vein disorders, offering patients in Northern Colorado and Southern Wyoming relief from the symptoms and appearance of troublesome veins. What is Endovenous Vein Ablation? Endovenous Vein Ablation is a minimally invasive procedure designed to treat varicose veins and other vein disorders. Unlike traditional surgical methods, which require large incisions and extensive recovery periods, endovenous ablation is performed using a catheter inserted into the affected vein. This catheter delivers controlled heat energy, sealing the vein shut and redirecting blood flow to healthier veins nearby. How Does It Work? During the procedure, your doctor will numb the treatment area and make a small incision to access the affected vein. A thin catheter is then inserted into the vein under ultrasound guidance. Once positioned correctly, the catheter delivers thermal energy, such as laser or radiofrequency, to heat and seal the vein. This process causes the vein to collapse and eventually be absorbed by the body, while blood flow is rerouted through healthier veins. Endovenous vein ablation can also be accomplished with chemical technolgoy, or with adhesives. At Total Vein Care, all of these approaches are utilized. Benefits of Endovenous Vein Ablation:
Is Endovenous Vein Ablation Right for You?
If you are experiencing symptoms of vein disorders such as varicose veins or spider veins, endovenous ablation may be an appropriate treatment option for you. However, it's essential to consult with a qualified vein specialist to determine the best course of action based on your individual needs and medical history. Contact us today to schedule an appointment in our Fort Collins office. At Total Vein Care in Fort Collins, our team of experienced vascular specialists is dedicated to providing personalized care and effective treatment options for patients in Northern Colorado and Southern Wyoming. We understand the impact that vein disorders can have on your daily life, and we are committed to helping you find relief through advanced treatments like endovenous vein ablation. Take the First Step Toward Healthier Veins Today! Don't let vein disorders hold you back any longer. Contact Total Vein Care in Fort Collins to schedule a consultation and learn more about how endovenous vein ablation can improve your vein health and overall well-being. With our expert care and innovative treatments, you can enjoy your freedom again.
0 Comments
We pride ourselves in offering our patients the highest quality care, in a personalized and professional environment. You’ll find the Total Vein Care staff; administrative and clinical, to be highly trained, friendly, and caring individuals who are concerned about the outcome and comfort of each and every patient.
Becky Juarez, Clinic Manager Becky has been a Registered Medical Assistant since 2010. She has managed the medical/surgical side of Total Vein Care since 2013. Becky hails from Pierce, Colorado. She and her husband have 3 sons and 2 dogs that keep her very busy. Her favorite pastime is watching her boys play baseball, football and wrestle! She is always cheering on her kids from the sideline of any sport they play! Mayra Aguirre, Front Desk Mayra is a Colorado native who has loved growing up in Fort Collins. She has 2 beautiful daughters that are her pride and joy! Mayra has been with Total Vein Care since 2018 and loves her job and the people she works with. She is the friendly voice that will help you schedule or answer your questions whenever you call and she is bi-lingual in Spanish as well. In her free time she like to spend time with her family and enjoying their company. Autumn Kendell, Medical Assistant Autumn has been a Medical Assistant since 2007 and she has worked with Total Vein Care since 2022. She is from a small town in Missouri and moved to Colorado with her husband of 13 years in 2021. They both love the mountains and being out in nature. In her time away from work she enjoys hiking, riding motorcycles and traveling! If you’re living with the discomfort of leg swelling in Fort Collins and Northern Colorado, Dr. Steven Kaufman and the team at Total Vein Care can help you find relief and treat the root causes.
Swelling of the legs can be caused by many factors, many of which fall into 2 categories: SYSTEMIC CAUSES These include problems such as heart failure, liver disease, or kidney disease. Fluid retention includes the above causes, but sometimes the cause is not known. The swelling is usually equal in both legs. VEIN AND LYMPHATIC CAUSES Causes of swelling in this group often include thrombosis (blood clots such as DVT), venous insufficiency caused by a failure of the valves in the veins, and lymphedema from obstruction of the lymphatic vessels. Lymphedema can be hereditary or the result of vein disease, injury, or surgery for cancer, where lymph nodes are often removed. In this group, the swelling is usually present in only one leg or worse in one leg than the other. Fluid Retention The second reason legs swell is because of edema or fluid retention in bodily tissue. In addition to the swelling, edema can cause your legs to change color, feel tight or heavy, itch, or feel numb. There are several things that cause fluid retention in the legs, some of which include:
Date: August 02, 2019
Contact: Tamara Sloper (sloper@intersocietal.org) PDF Press Release: Download it here Total Vein Care Earns Vascular Testing Reaccreditation by the IAC Early detection of life threatening heart disorders, stroke and other diseases is possible through the use of vascular testing procedures performed within hospitals, outpatient centers and physicians’ offices. Cardiovascular diseases are the No. 1 cause of death in the United States. On average, one American dies every 39 seconds of cardiovascular disease – disorders of the heart and blood vessels. Stroke, a disorder of the blood supply to the brain, is the third leading cause of death and the leading cause of disability in the country, with nearly 800,000 new strokes occurring annually. There are many factors that contribute to an accurate diagnosis based on vascular testing. The training and experience of the technologist performing the procedure, the type of equipment used and the quality assessment metrics each facility is required to measure, all contribute to a positive patient outcome. IAC accreditation is a “seal of approval” that patients can rely on as an indicator of consistent quality care and a dedication to continuous improvement. Total Vein Care located in Fort Collins, CO has been granted a three-year term of accreditation by the Intersocietal Accreditation Commission (IAC) in Vascular Testing in the area(s) of Peripheral Venous Testing. This latest accreditation awarded to Total Vein Care demonstrates the facility’s ongoing commitment to providing quality patient care in vascular testing. Accreditation by the IAC indicates that Total Vein Care has undergone an intensive application and review process and is found to be in compliance with the published Standardsthus demonstrating a commitment to quality patient care in vascular testing. Comprised of a detailed self-evaluation followed by a thorough review by a panel of medical experts, the IAC accreditation process enables both the critical operational and technical components of the applicant facility to be assessed, including representative case studies and their corresponding final reports. About IAC IAC provides accreditation programs for vascular testing, echocardiography, nuclear/PET, MRI, diagnostic CT, dental CT, carotid stenting, vein treatment and management and cardiac electrophysiology. The IAC programs for accreditation are dedicated to ensuring quality patient care and promoting health care and all support one common mission: Improving health care through accreditation .IAC accreditation is widely respected in the medical community, as illustrated by the support of the national medical societies related to vascular testing, which include physicians, sonographers and technologists. To date, the IAC accrediting divisions have granted accreditation to more than 14,000 sites throughout the United States, Canada and Puerto Rico. In Fall 2018 Dr. Kaufman presented a 2-hour lecture series at the University of Northern Colorado speaking on the the topic of Venous and Lymphatic Medicine for the Family Nurse Practitioner Program at the UNC School of Nursing.
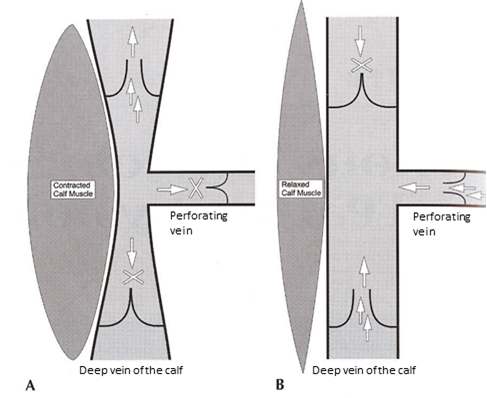
We all hear about the beneficial effects of exercise on the cardiovascular system. “Cardio” makes the heart more efficient. Exercise, in general, elevates HDL cholesterol which in turn slows the development of atherosclerotic plaque in the coronary arteries, thus lessening the risk of heart attack. Very few of us discuss the beneficial effects of exercise on the venous system. The veins in the lower extremities receive blood from the muscles and deliver it to the heart. The blood is then pumped to the lungs where it receives oxygen to nourish the organs and muscles in the body. The veins have a tough job. Unlike arteries which have the benefit of gravity and the heart for pumping their blood down into the legs, veins do not benefit from the constant pumping action and have to fight gravity to move their blood up to the heart. In people with healthy veins, a series of one-way valves prevents the blood from settling down into the feet and ankles. Unfortunately, many people have valves that do not function properly, causing a condition known as venous insufficiency. Venous insufficiency causes symptoms such as aching, heaviness, and fatigue of the legs. In more severe cases this process damages the skin, leading to darkening, thickening, and even ulceration of the skin just above the ankles. So, how do the veins do it? Their blood receives its propulsion from contraction of the calf muscles, the gastrocnemius and soleus muscles. Phlebologists (experts in diseases of the veins) refer to this as the calf muscle pump, figure 1). This mechanism is so efficient that one contraction of the calf propels 60% of the blood in the leg toward the heart. 10 to 20 contractions decrease the pressure in the lower leg veins from 100mmHg to 20mmHg in a matter of seconds. Interestingly, many with venous insufficiency find that their symptoms improve soon after they begin walking or performing any exercise that results in contraction of the calf. With reduction of the pressure in the veins with exercise, the legs no longer ache or feel heavy. With regular continuous exercise such as walking, running, cycling, or use of an elliptical trainer or stair-stepper for 30 minutes a day can make the legs feel much better. With age or development of a neuromuscular disease, atrophy of the calf muscles can occur, resulting in the symptoms and sometimes the skin problems associated with venous insufficiency. People with atrophy of the calf muscles can benefit from exercises designed to strengthen them. Calf raises and dips while standing with the forefoot on a step can strengthen the calf muscle pump and reduce the effects of venous hypertension. If you want to be good to your veins, try 30 minutes of continuous exercise each day and exercise the calf muscles to keep them strong. Dr. Steven Kaufman is Board Certified in Surgery and Venous and Lymphatic Medicine. He practices at Total Vein Care, 1136 East Stuart Street, Suite 4102, Fort Collins, CO 80525. He can be reached at (970) 498-8346 or on the web at totalvein.net.
|
AuthorDr. Steven Kaufman is a board-certified surgeon and phlebologist specializing in the diagnosis and treatment of vein disorders. He is Northern Colorado’s leading vein care specialist, with the education, experience, advanced training, and positive patient outcomes to make him the preferred choice for the care of your vein problem. Archives
April 2024
Categories |
Total Vein Care - Vein Specialist in Northern Colorado
Total Vein Care is honored to be accredited and associated with the leading partners in our industry.
|
Total Vein Care
1136 E Stuart Street, Suite #4102 Fort Collins, CO 80525 (970) 498-8346 info@totalvein.net |
Get In Touch:
Open Monday - Friday: 8 am - 5 pm
|
Website by Canopy Creative Marketing. Copyright © 2020. Total Vein Care . All Rights Reserved. Privacy Policy.