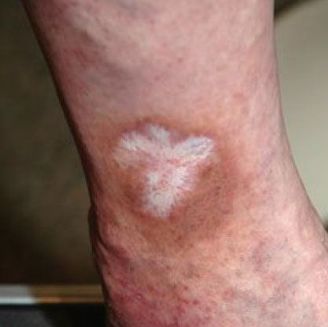
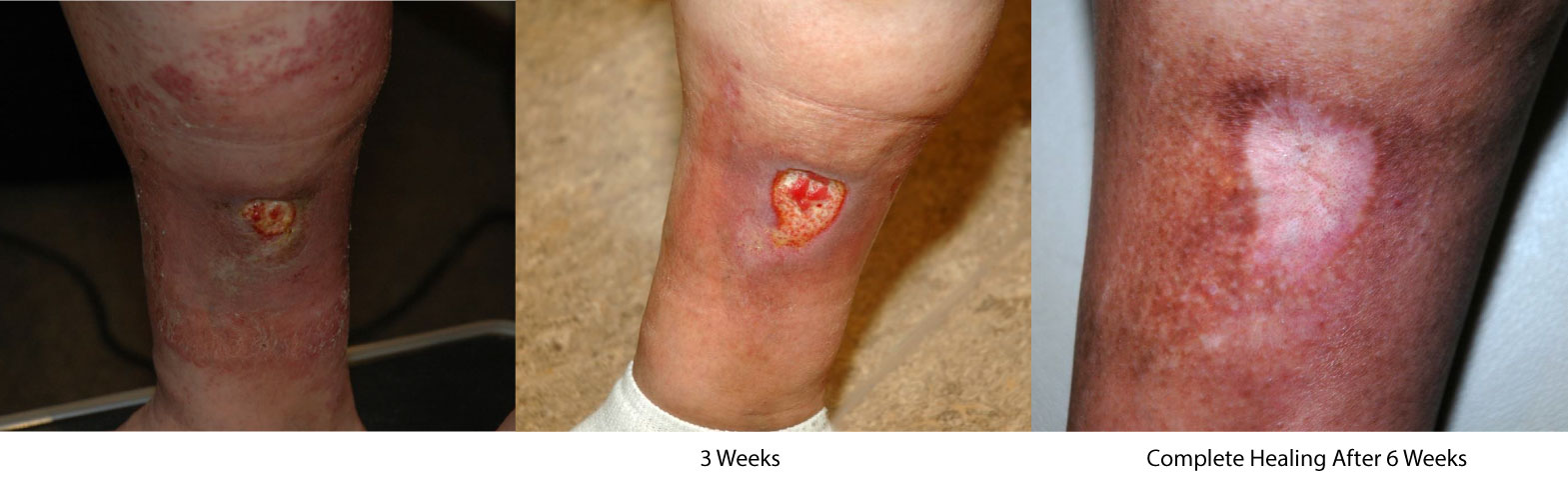
The skin is the end of the line when it comes to damage from venous hypertension. The early stages of chronic venous insufficiency include spider veins, varicose veins, and leg swelling. The more advanced stages, C4-6 in the classification system, all involve the skin. The mechanisms through which venous hypertension causes skin damage are complex and not well understood. Regardless, the pattern of progression is consistent. Initially, the skin develops a brownish darkening of the skin (hyperpigmentation) near the ankle, although it often involves a larger area. Eczema, an inflammation of the skin producing flaking or scaling, also develops early in the process. Later, the inflammation progresses and the skin hardens from scarring and fibrosis, a finding we referred to as lipodermatosclerosis. As the damage to the skin advances, whitish areas of skin develop, and these are referred to as atrophie blanche. Scars of healed ulcers may have a similar appearance. Finally, an active ulcer, involving the full thickness of the skin, develops and fails to heal, sustained by CVI. Venous ulcers usually form between the lower edge of the calf muscle and the ankle, making them easy to distinguish from diabetic ulcers and other types of wounds.
|
Venous leg ulcers (VLU) account for 70% of all leg wounds. Approximately 20% of people who suffer with chronic venous insufficiency develop leg ulcers. In the US, the cost of treating these wounds is approximately 1% of the healthcare budget, roughly $2.5 billion per year, in more than 6 million patients. In an outpatient setting, the direct cost of treating venous leg ulcers is estimated to be at least $2,500 per month, incorporating facility (wound clinic), physician, labor (i.e., nurses), medication, wound dressing, and compression garment costs. There are additional costs associated with treating the chronic venous insufficiency which underlies development of venous leg ulcers. These costs are quite low in comparison to the direct costs of treating the wounds, especially when they involve the superficial veins.
|
A set of guidelines for treating venous leg ulcers has been established through the cooperation of the Society for Vascular Surgery and the American Venous Forum. The guidelines include:
It has been clearly shown that adherence to these guidelines results in faster healing and a lower rate of ulcer recurrence. Because the underlying cause of these wounds is venous disease, this must be treated early in the course of therapy. Failure to do so results in unnecessary expense and loss of work days by patients. Without correction of CVI, wound care can require months, or even years, of very costly treatments. Correction of the underlying venous disease can lead to rapid healing of an ulcer and reduced likelihood of an occurrence. At the time referral to a wound clinic for a leg wound in the location typical for a venous ulcer, consultation by a venous disease specialist should be requested.
- Compression therapy, for healing a wound and prevention of recurrence
- Wound care and dressings
- Medications
- Surgical correction of chronic venous insufficiency
It has been clearly shown that adherence to these guidelines results in faster healing and a lower rate of ulcer recurrence. Because the underlying cause of these wounds is venous disease, this must be treated early in the course of therapy. Failure to do so results in unnecessary expense and loss of work days by patients. Without correction of CVI, wound care can require months, or even years, of very costly treatments. Correction of the underlying venous disease can lead to rapid healing of an ulcer and reduced likelihood of an occurrence. At the time referral to a wound clinic for a leg wound in the location typical for a venous ulcer, consultation by a venous disease specialist should be requested.